CMI has developed a proprietary revenue cycle process which ensures maximum reimbursement for our clients. This process maximizes the quality, efficiency, and cost-effectiveness of the anesthesia billing services we provide.
Most of our competitors use inexperienced, offshore resources resulting in a tremendous amount of revenue being left in the pockets of the insurance companies.
CMI integrates a perfect blend of automation and personal involvement to go way beyond picking only the low hanging fruit!
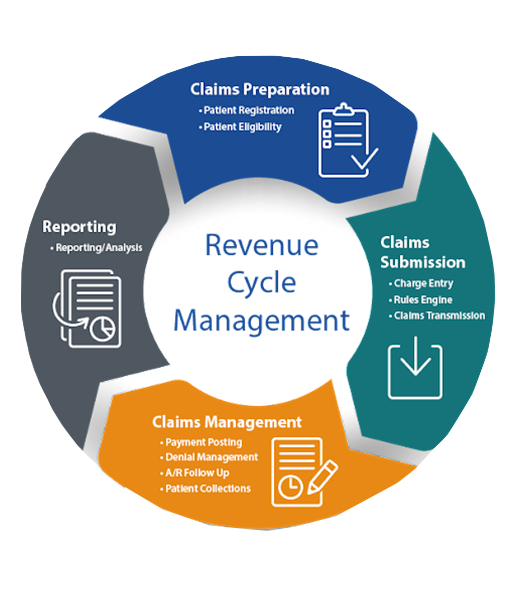
Preparation
Our clients range from sole practitioners to large, hospital-based anesthesia groups (and everything in between). Whether you’re charting by paper or utilize an Anesthesia Information Management System, we customize a solution to ensure seamless integration with little to no change to your current workflow.


Submission
Following receipt of your billing data, whether in digital or paper format, claims are generated by our team of Certified Coders. All documentation is thoroughly reviewed to ensure that all billing opportunities are captured, maximizing the income potential. CMI’s Deductible Hold feature checks insurance policy accumulators each night. Clients have the option to hold claim submission until deductibles or maximum out-of-pockets are met. If the threshold is not met prior to timely filing, the claim will automatically be released to avoid denial. It's easier to collect money from an insurance company than it is from a patient!
Claims Management
Any billing company can transmit anesthesia claims and record payments. The real work only begins after the claim is adjudicated by the insurance company. Our process of addressing claim denials and underpayments produces clear and measurable results.
In-Network Claims:
Our billing platform reconciles every payment against your pre-loaded Managed Care Fee Schedules. Any deviation in reimbursement is flagged for our team to address and appeal. Assuming the payment is consistent with the fee schedule, any cost sharing is billed to the patient the very same day.
Out-of-Network Claims:
The Federal No Surprises Act (NSA) was passed in December of 2020, but it only recently became effective on January 1, 2022. It aims to protect patients from receiving surprise bills, though it also gives insurers the upper hand if your practice is not intimately familiar with the ever-evolving arbitration process. Since anesthesia groups are no longer permitted to balance bill their patients, insurers have begun slashing out-of-network reimbursement to unprecedented levels. Healthcare experts believe that many anesthesia providers will be strong-armed into going in-network at very low rates to avoid even lower out-of-network reimbursements.
By leveraging CMI's resources and expertise, your out-of-network practice will remain very lucrative! The days of appealing poorly paid or denied claims because "the patient didn't have a choice" or "the surgeon was in-network" are long over. Today, appeals have evolved into a more complex, time-sensitive process. CMI has prevailed in hundreds of arbitrations and handles each claim individually by:
- Properly initiating the negotiation process in the required time frame
- Negotiating with payers and third-party re-pricing firms during the 30-day window
- Triggering the arbitration process within 4 days over the negotiation period through the appropriate state/federal portal
- Bolstering our arbitration package with substantive data that aims to bypass the Qualified Payment Amount
Failure to give the process personal attention to detail will make or break your case!
Reporting
Recognizing the importance of meaningful data, CMI has developed a variety of standardized reports to illustrate the financial health of your practice. Whether you’re negotiating managed care contracts or analyzing staff utilization, our reporting options allow you to drill down to even the most granular details of your business. If one of our reports doesn’t quite show what you’re looking for, we’re happy to create a custom report which will! With the best reporting capabilities, strategic partnerships, and personalized service, CMI will ensure that your practice stays on track and collects the most revenue possible.

